Alan talks about the pioneering project helping patients get the post-treatment support they need - moving patient representation from involving to demonstrably influencing and delivering transformational change throughout cancer networks across Scotland.
More people than ever before are surviving a cancer diagnosis but at the same time incidences of cancer are increasing. By 2030, the number of people living with cancer in Scotland is expected to rise from 220,000 to 360,000 (Macmillan Cancer Support). Thus, health services need to consider how care and support are delivered after treatment.
For this reason, Macmillan Cancer Support – in partnership with NHS Scotland and The Scottish Government – have invested £5 million in the Transforming Care After Treatment (TCAT) programme. This recognises that cancer care should not stop when treatment ends but continue until the individual no longer needs support.
Transforming Care After Treatment
The TCAT programme is a five-year initiative which started in 2013. It has a Scotland-wide agenda to transform care and provide an exemplary model of integration. The programme involves the integration of the NHS, health and social care, and third sector groups to make the best use of resources.
Although increasing cancer survival rates are positive, many patients are left experiencing a range of problems after the all-clear, from the physical and emotional to the financial and practical.
Putting people first
TCAT is a unique programme of work, one of the largest of its kind in the UK. What is also unique is the strong influence of those with lived experience throughout its delivery. These people are helping shape the delivery of multiple work streams across the three key phases.
From the outset, the creation of the Cancer Experience Panel (CEP) to represent these voices was seen as fundamental to its success, offering a new model of integration. The CEP has a clear authority and has been given an equal share in the decision-making process. For example, they had 50% of the ‘votes’ that decided on the allocation of TCAT funding to projects. More importantly, the CEP ensures the programme is improving experiences for people with cancer by involving them and guarantees their voices are listened to.
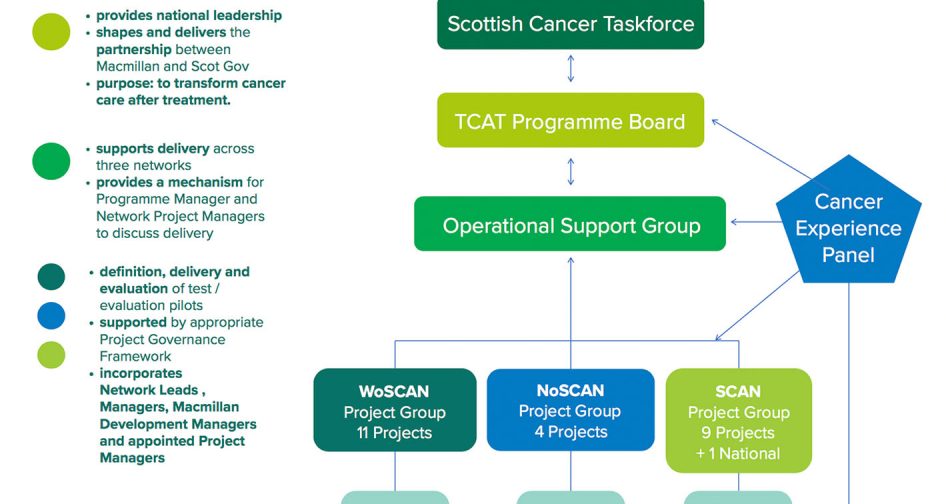
Image created by Alan Ainslay
The voice of Gill
To date, there have been many significant and emotional times when people living with cancer have shared their experiences and made a profound impact on services and professional practice in Scotland.
The voice of Gill, a mother and a dear friend who, despite her terminal diagnosis, made a significant contribution to the Midlothian Living Well After Treatment project by suggesting services help the children of cancer patients. Her ideas were gratefully listened to and acted upon by the wonderful people at Midlothian District Council.
Taking on this kind of responsibility can be difficult whilst coping with the burden of illness and prolonged treatments. Still, it has been important for all members of the Cancer Experience Panel (CEP) and other active patient/user groups to understand how vital their role has become in producing better services.
These voices of experience have been listened to. Their ideas and thoughts acted upon.
Each voice has offered a personal pathway of lived experience and of shared experiences. And because no two stories are the same, they have been an invaluable resource, now mined for all they’re worth.
These people understand the impacts of treatment cycles. They understand that even if the cancer is beaten, its memory lives with you forever, in your mind and/or physically through the after-effects of treatment. The fear of it returning never goes away.
The Cancer Experience Panel
Apart from scrutinising results from TCAT projects and other reforms to see if all the concerns of people with cancer are addressed, the CEP can see if the different health and social care services are joined up and provide co-ordinated, well-timed care and support.
As we enter the final phase of TCAT, with less than 18 months of the programme remaining, the role of CEP is more important than ever.
The focus is now on how to spread and embed the learning from the first two phases of the project and help drive this through the Regional Cancer Networks.
Key learning themes include the introduction and spread of Holistic Needs Assessments and the introduction of End of Treatment summaries.
At a political level, the CEP and its members in networks and projects now have the evidence of performance to prove how involving these voices delivers demonstrable results of positive, transformational change.


The best & worst
We are currently in the best and worst time to reform Scottish public services and to improve life for people with cancer.
It’s the best time because we have clarity about what needs to be done in terms of strategy, research and outcomes. However, it’s the worst time because we have the coldest financial climate in decades and the highest levels of demand on health and social care.
Focus on what the individual needs, not what the individual wants
I feel fortunate to have seen first-hand the power of the voices of experience: how they have been listened to; how they have represented these different experiences, and; how they have helped transform services – working in tandem with health professionals, for the good of everyone.
These voices have supported local service user reference groups and provided representation at a regional level. They have promoted the value of service user involvement at every level. Furthermore, they have represented and empowered service users to take a role in strategic decision-making and care planning.
In one of the Phase 1 projects, these voices contributed to the effective transition from acute care at the end of active treatment back to the community setting. Utilising the holistic needs assessment, a questionnaire designed by the multidisciplinary team responsible for the bid.
In one of the Phase 2 projects, these voices helped enable people to live as independent a life as possible within their own communities following their diagnosis of cancer. A re-ablement approach is being used to ensure that their functional skills and confidence could be retained or regained, to enable them to participate in their everyday activities.
For me, what is most impressive is the model itself. This is service design at its best. Person-centred care designed by the people using the services. Throughout, it has focused on what matters most to the individual – meeting needs, not wants.
Alan Ainsley is a Partner at Snook and also Deputy Chair of the Cancer Experience Panel.
*Phase 1 – 11 Projects, one in the Highlands, the remainder across the central belt and the borders. Bids were led by Health Boards. Focus on needs assessment and care pathway improvements.
** Phase 2 – 15 Projects, from the borders to Inverness. Bids led by local authority partners – less clinical, more social. Focus on self-management and ongoing, more individualised support.
All projects were instructed to develop a partnership approach with patients as part of their development and management.
